Shingles
Symptoms, common medications, and savings
Loading...
Medically reviewed by Carina Fung, PharmD, BCPPS on June 1, 2020
What is shingles?
Shingles[1], also known as the zoster virus or herpes zoster virus, is a skin rash and nerve disease[2] caused by the reactivation varicella-zoster virus (VZV, the same virus that causes chickenpox). Although shingles isn't usually contagious, it can be spread from an infected person to someone without immunity to chickenpox. More commonly, however, singles is caused by the re-emergence of the chickenpox virus.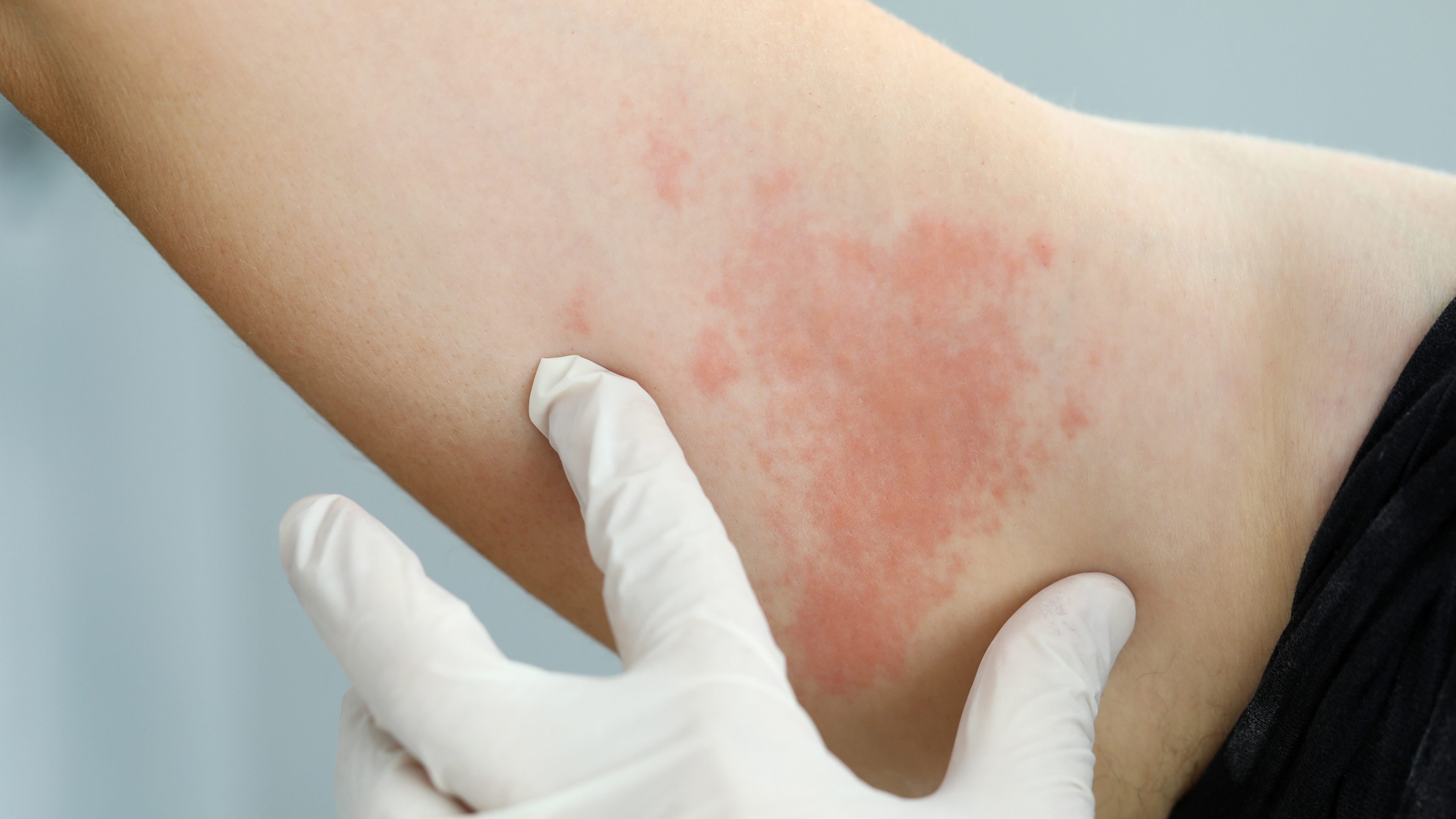
Source: Getty Images
How common is shingles?
One in every three people in the United States[4] will get shingles at some point in their life. It is estimated that one million cases of shingles are diagnosed in the United States each year. The incidence rate[5] of shingles across the United States’ general population is 4 cases per 1,000 people. In people over the age of 60, however, this rate is 1 case per 100 people. According to the United States National Institutes of Health, the incidence of shingles is on the rise. This may be attributable to increasing life expectancies, as people who live to be 85 years old have a 50% chance[6] of developing shingles.What causes shingles?
Shingles is caused³ by the same virus that causes chickenpox, known as the varicella-zoster virus (VZV). Once chickenpox has resolved, the virus can enter the nervous system and remain in the body in a dormant, or inactive, state. Over time, VZV can reactivate and travel to the skin along the body’s nerve pathways. This is what causes shingles. Anyone who has had chickenpox is susceptible to getting shingles. However, not everyone who has had chickenpox in the past is guaranteed to develop shingles. Ultimately, it’s still unclear as to why some people develop the disease. It has been supposed that shingles may result from weakened resistance (immunity) to infections, as the disease is more common in older adults and those who are immunocompromised (have weakened immune systems). VZV is included in the herpes family of viruses. Despite this, the virus is not responsible for oral herpes (HSV-1) or genital herpes (a sexually transmitted infection most commonly caused by HSV-2).Is shingles contagious?
Shingles can be contagious[7], in some cases. If you have shingles, it’s possible for you to pass it to someone else who has not developed immunity to chickenpox. People without immunity to the disease include those who have never had chickenpox, including newborn children, and those have not received the chickenpox vaccine. When shingles is passed from person to person, it typically occurs as the result of direct contact with the open blisters characteristic of the shingles rash. This is why if you have shingles, you should avoid coming into close contact with anyone who may not have immunity to chickenpox until after your blisters have hardened or scabbed over. It is also advised that you avoid contact with women who are pregnant if you have shingles.Risk factors for shingles
Certain factors, including pre-existing conditions, may increase the risk[8] of developing shingles, including[9]:- Prior viral infection: Anyone who has had chickenpox is at risk of developing shingles. This is a large part of the population, as nearly all people born in the United States before 1980[10] had chickenpox as a child.
- Chickenpox vaccination: If you were immunized to chickenpox at some point in your life, you are still at risk of developing shingles. However, that risk is significantly lower than if you had chickenpox as a child.
- Age: While shingles is most common in people over the age of 50, the risk of developing the disease increases with age.
- Cancer: Cancer treatments typically involve chemotherapy and radiation, both of which can weaken the immune system and decrease the body’s ability to fight off infections.
- HIV/AIDS: Both HIV and AIDS weaken the immune system. People who are immunocompromised (have weakened immune function) are known to have an increased risk of developing shingles.
- Receiving an organ/bone marrow transplant: Bone marrow transplant and organ transplant recipients must take immunosuppressive medications to help prevent the new tissues from being rejected. As with cancer treatment and HIV/AIDS, this lowers the immune system’s function and increases the risk of shingles.
- Taking immunosuppressants: Medications and treatments that suppress your immune system, such as steroids and chemotherapy, may increase your risk of developing shingles. People with autoimmune diseases, such as systemic lupus erythematosus (SLE) or rheumatoid arthritis, often take these medications, increasing their risk of developing shingles.
- Biological sex: Women have been found to develop shingles more frequently than men, though the cause of this discrepancy is unknown.
- Race: Caucasians are two times more likely to get shingles than people of other races and ethnicities (specifically African Americans).
Shingles symptoms
The initial symptoms of shingles may resemble those of other conditions with associated skin rashes. Before sores start to form, however, a person with shingles may feel parts of their skin become itchy, numb, tingly, or painful. They may also experience sensitivity to sunlight or bright lights (photosensitivity), fatigue, or headaches. Once the characteristic shingles rash develops, it usually affects only a small area or remains localized to one side of the face or body. Shingles rashes commonly develop around the waist on one side or the other, as well as on the face or ears. Some common signs[11] and symptoms[12] of shingles include:- Sensations of itching, burning, or tingling on the skin preceding any rashes or blisters
- Skin sensitivity
- Blister-like sores, sometimes filled with fluid
- Fever
- Chills
- Stomachache
- Headache
- Swollen lymph nodes
- Joint pain
Shingles rash
The rash caused by shingles often presents itself at first with redness. Some people with shingles experience this redness accompanied by burning, tingling, numb, or itchy skin. Shingles sores (called lesions) typically begin to form within one week of the onset of initial symptoms. These lesions usually appear as clusters of small red pustules[13] that may be fluid-filled. These fluid-filled blisters often burst. Once a blister bursts, the area around it may start to dry out and become crust-like. These dried blisters usually fall off naturally within two to three weeks and rarely cause permanent scarring. Shingles or herpes zoster sores typically occur[14] on the abdomen or back and usually affect just one side of the body. This form of the rash, which occurs when lesions arise in one or two nearby areas of the body, is known as localized zoster. Sores that are more widespread are referred to as disseminated zoster. Disseminated zoster sores usually only occur in people who are immunocompromised. While it is uncommon for shingles sores to cause lasting scars, it may still happen depending on the severity of the sores and how long you wait before seeking treatment.Complications from shingles
Even after your shingles rash resolves, the virus has the potential to cause other complications[15]. It is estimated that 1–4%[16] of people with shingles will be hospitalized for complications related to the herpes zoster virus. Of those who are hospitalized for shingles complications, 30%¹² are immunosuppressed or immunocompromised. Some potential complications from shingles include:- Postherpetic neuralgia (PHN): PHN, a common complication of shingles, is characterized by lingering pain in the area where the shingles rash once was. In order to be classified as PHN, this pain must continue for at least 90 days after the rash first began.
- Herpes zoster ophthalmicus: Shingles virus that arises in the eye area is known as herpes zoster ophthalmicus.[18] This condition may involve a forehead rash or tissue inflammation of the eye and its surrounding area.
- Bacterial infection: In some cases, shingles lesions can become infected (often with the bacteria Staphylococcus aureus).
- Cranial or peripheral nerve palsy (Ramsay Hunt syndrome[19]) : When varicella zoster or herpes zoster is reactivated in the area surrounding the facial nerves, it can lead to a condition known as Ramsay Hunt syndrome (RHS). RHS is associated with facial paralysis, rashes around the ears or mouth, and, in some cases, hearing loss or ringing in the ears (tinnitus).
- Herpes zoster encephalitis (HZE)[20]: In rare cases, shingles can arise in the cranial nerves and lead to neurological complications, such as swelling of the lining of the brain.
- Pneumonitis: A complication known as pneumonitis[21], or lung tissue inflammation, occurs in roughly 5–10% cases of herpes zoster. Pneumonitis is associated with lung-related symptoms, such as coughing, shortness of breath, and fever. In patients who develop pneumonitis, these symptoms usually start within one week of developing the shingles rash.
- Hepatitis: Liver failure due to inflammation (hepatitis[22]) may occur in some patients with disseminated herpes zoster (shingles that has spread to three or more areas of the body).
- Acute retinal necrosis: People who are immunocompromised are at an increased risk of developing a complication known as acute retinal necrosis[23], or tissue death of the retina (a part of the eye).
Medications
Related Conditions
Chickenpox
A highly contagious viral infection that causes an itchy, blister-like rash on the skin....
Rosacea
A common, long-term condition that can affect the face and the eyes. It causes redness, visible blood vessels, and, in s...
Pneumonia
Lung inflammation caused by a bacterial or viral infection in which air sacs fill with pus. In severe cases, pneumonia c...
Diabetic Nerve Pain
Diabetic nerve pain is a type of nerve damage that occurs in people with diabetes. This damage makes it hard for nerves ...