Diabetic Nerve Pain
Symptoms, common medications, and savings
Loading...
Medically reviewed by Carina Fung, PharmD, BCPPS on December 27, 2019
What is diabetic nerve pain?
Diabetic nerve pain, also called diabetic neuropathy[1], is a type of nerve damage that occurs in people with diabetes. This damage makes it hard for nerves to carry messages to the brain and other parts of the body. High blood sugar (glucose) levels can injure the nerves throughout your body. Having high blood sugar, or hyperglycemia, for extended periods of time increases your likelihood[2] of getting nerve damage. The nerves in the feet are usually the first to be damaged by hyperglycemia. If you notice any pain or loss of feeling in a specific part of your body, your healthcare provider can conduct or order testing to help you determine the cause. Depending on what nerves are affected, diabetic nerve pain can also impact the function of your heart, blood vessels, digestive system, and urinary tract. Some people with diabetic nerve pain have mild symptoms, while for others, the condition can be disabling.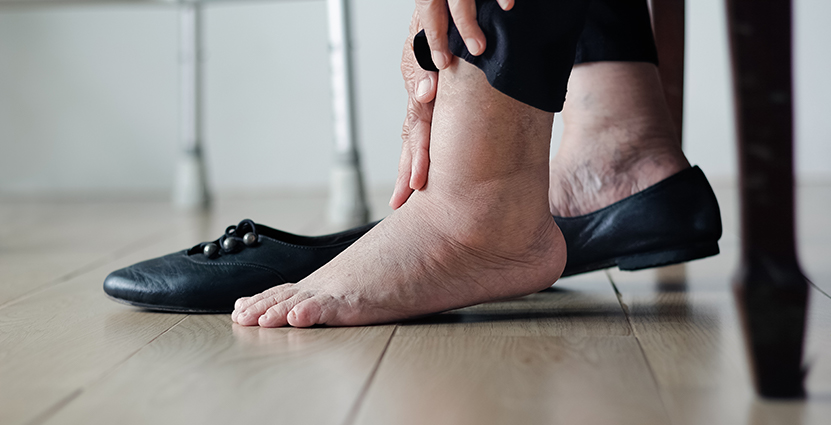
Source: Getty Images
Diabetic nerve pain causes
Research indicates that high blood sugar levels[5] damage nerves over time[6] by interfering with their ability to send signals. Having hyperglycemia also weakens the walls of the small blood vessels (capillaries) that supply the nerves with oxygen and nutrients. This damage is what leads to diabetic nerve pain. Other factors that can lead to diabetic nerve pain include an autoimmune response to the nerves, genetic factors, smoking, and excess alcohol consumption. Anyone with diabetes can develop nerve pain, particularly if they have had diabetes for a long time. Other factors that increase the likelihood of developing nerve damage include:- Poor blood sugar control, which increases the risk of all diabetes-related complications, including nerve damage.
- Kidney disease, which can cause toxins to be released into the blood, leading to nerve damage.
- Being overweight. Your risk of getting diabetic nerve pain is higher if you have a body mass index (BMI) greater than 24.
- Smoking, which reduces blood flow to the extremities (limbs, hands, and feet) by narrowing and hardening the arteries. When blood flow is decreased, wounds take a longer time to heal, increasing the likelihood of your peripheral nerves being damaged.
Complications from diabetic nerve pain
Diabetic nerve pain can lead to a number of health complications, depending on which nerves are affected. These include:- Infection: Having diabetic nerve pain in your feet puts you at a greater risk of developing infections in sores or cuts. In severe cases, infections can spread to the bones and lead to tissue death (gangrene), which can potentially require amputation.
- Joint damage: Nerve damage can cause the joints to deteriorate—especially the small joints in the feet. The symptoms of joint damage include loss of sensation, joint swelling, instability, and, in some cases, joint deformity. Prompt treatment is necessary to help you heal and prevent further joint damage from occurring.
- Urinary tract infections: When the nerves that control your bladder are damaged, you may not be able to fully empty your bladder or control your urination. This can cause bacteria to build up in the bladder and kidneys, potentially leading to urinary tract infections.
- Undetected hypoglycemia: If you have autonomic neuropathy, you may not notice the warning signs of low blood sugar, which include shakiness, sweating, and a fast heartbeat.
- Hypotension: It’s harder for your body to regular your blood pressure when the nerves that control blood flow are damaged. This can lead to hypotension, or low blood pressure. One common symptom of hypotension is feeling dizzy when you stand after sitting.
- Digestive problems: Nerve damage in your digestive tract can lead to constipation, diarrhea, and other digestive complications.
- Sexual dysfunction: Nerve damage to in the sex organs can lead to decreased self-lubrication in women and erectile dysfunction in men.
- Irregular sweating: Nerve damage can disrupt how your sweat glands function. You might sweat too much or too little, making it harder for your body to properly regulate its temperature.
Diabetic nerve pain symptoms
The symptoms of diabetic nerve pain develop gradually. You may not notice anything is wrong until considerable nerve damage has already occurred. The symptoms you experience will depend on which nerves are affected. There are four types of diabetic neuropathy: peripheral, autonomic, radiculoplexus, and focal neuropathy. Peripheral neuropathy is the most common form of diabetic neuropathy. This form of the condition first affects the feet and legs, followed by the hands and arms. The signs of peripheral neuropathy are often worse at night, and may include:- Numbness or a reduced ability to feel pain or temperature changes
- Tingling or burning sensations
- Sharp pains or cramps
- Increased sensitivity to touch
- Weak muscles
- Loss of balance, coordination, or reflexes
- Foot problems such as ulcers, infections, and bone and joint pain
- Changes how your eyes adjust from light to dark
- Quickened heart rate at rest
- Sharp drops in blood pressure after sitting or standing that makes you feel lightheaded
- Slow stomach emptying causing nausea, bloating, or loss of appetite
- Constipation or diarrhea
- Difficulty swallowing
- Not knowing that blood sugar levels are low (undetected hypoglycemia)
- Bladder problems, including incontinence or urinary tract infections
- Irregular sweating and problems controlling body temperature
- Erectile dysfunction
- Vaginal dryness
- Decreased sexual response
- Pain in your hip, thigh, or buttocks that occurs for one or more days
- Difficulty rising from a sitting position
- Abdominal swelling, if the abdomen is affected
- Weight loss
- Eventually, weak and shrinking thigh muscles
- Shin or foot
- Lower back or pelvis
- Front of the thigh
- Chest or abdomen
- Difficulty focusing
- Double vision
- Aching behind one eye
- Paralysis on one side of the face
Medications
Related Conditions
Type 2 Diabetes
Diabetes Milletus
A chronic condition that affects the way the body metabolizes sugar (glucose). Develops when the body becomes resistant ...
Type 1 Diabetes
Diabetes Milletus
A chronic autoimmune condition in which the pancreas produces little or no insulin....
Prediabetes
A condition in which your blood sugar (glucose) levels are higher than normal but not yet high enough to be classified a...
Chronic Pain
A sharp or dull pain that lasts at least 12 weeks, and which may cause a burning or aching sensation in the affected are...