High Cholesterol
Symptoms, common medications, and savings
Loading...
Medically reviewed by Carina Fung, PharmD, BCPPS on October 1, 2019
What is high cholesterol?
High cholesterol, also known as hypercholesterolemia or hyperlipidemia, is a condition in which the body’s cholesterol levels are elevated beyond what is healthy and necessary for normal function.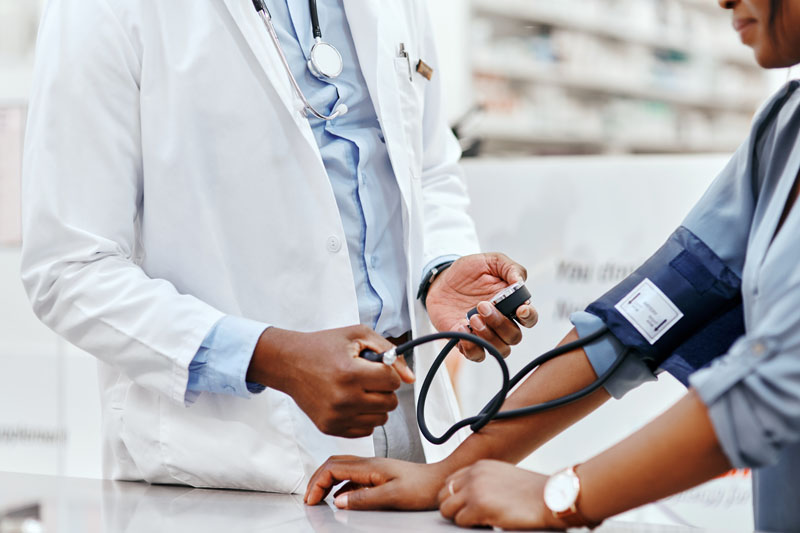
Source: Getty Images
- The narrower arterial passages present an increased likelihood of thrombosis (i.e., a blood clot becomes stuck and obstructing blood flow).
- A piece of plaque buildup can detach itself from the blood vessel wall and get stuck elsewhere in the bloodstream.
What are high cholesterol symptoms?
While high cholesterol is a serious condition, it typically produces few, if any, outward physical symptoms. Many patients may show no obvious external signs of high cholesterol, even at significantly elevated levels. In some individuals with extremely high cholesterol levels, yellow fatty deposits may be observable in the skin around the eyes (xanthelasmas) or over the tendons (xanthomas). Additionally, a phenomenon known as arcus senilis[7]—fat deposits in the eyes manifesting as a gray or white arc above and below the cornea—can be indicative of particularly severe cases of familial hypercholesterolemia in younger people. Note that this is not necessarily symptomatic of high cholesterol at age 45 and older, as arcus senilis is common in older adults.What else to look out for
Given hypercholesterolemia’s comorbidity with other conditions, even in the absence of symptoms, other more outwardly observable conditions can potentially point to high cholesterol (or at least a heightened risk for it). These include:- Diabetes
- Hypothyroidism
- Cardiovascular disease
- Nephrotic syndrome
- Cholestasis
- What is your dietary intake? If a large proportion of the calories you consume come from saturated fats, trans fats, or foods high in dietary cholesterol, you run a higher risk of elevated “bad” LDL cholesterol levels.
- Do you exercise regularly? Lack of sufficient physical activity can result in suboptimal levels of “good” HDL cholesterol.
- Are you a smoker? Smoking increases the harmful effects of high cholesterol, and may even negatively impact cholesterol levels themselves.
Causes of high cholesterol: lifestyle vs. genetics
The causes of high cholesterol[3] can be myriad: genetics, lifestyle choices, and other medical conditions can all potentially play a role. Behaviors that can cause or exacerbate high cholesterol include:- Diet: Consumption of foods high in saturated fats (found in meat and other animal products as well as tropical oils such as palm oil and coconut oil) and trans fats (often found in commercially packaged and processed foods) is associated with increased cholesterol levels. Additionally, foods high in dietary cholesterol (red meat and full-fat dairy products) will raise cholesterol levels.
- Sedentary lifestyle: Exercise helps the body produce “good” cholesterol (high-density lipoprotein), which in turn helps to mitigate the negative effects of “bad” cholesterol (low-density lipoprotein). Getting little or no exercise forgoes this benefit to good cholesterol levels, worsening the impact of bad cholesterol.
- Smoking: Smoking causes damage to the tissue lining the walls of arteries and other blood vessels. This makes it easier for plaque deposits induced by high cholesterol to build up within the circulatory system. Additionally, smoking might also lower good cholesterol levels.
How common is high cholesterol?
Because of the often complex interaction of inherited and behavioral risk factors, the rate of high cholesterol can vary—sometimes significantly—depending on the population. The CDC reports that more than 73 million adults in the U.S. have high cholesterol. Certain ethnic backgrounds (e.g., French-Canadian, Lebanese, Afrikaner) show a disproportionately high prevalence of familial hypercholesterolemia, with some data on these populations suggesting a rate as high as 1 in 100 compared to the baseline average of 1 in 250.LDL and HDL Cholesterol: What’s the difference?
Understanding the testing[5], diagnosis, treatment and effects of high cholesterol requires becoming familiar with the two main types of cholesterol[6]: low-density lipoprotein (LDL) and high-density lipoprotein (HDL). What’s the difference between these two substances that occur naturally in the body? Healthcare providers often distinguish the two from each other as “good” (HDL) cholesterol and “bad” (LDL) cholesterol. While the body requires and naturally produces both types, they have markedly different physiological effects. Most of the cholesterol in the body is made up of LDL, which delivers cholesterol to peripheral tissues, where it is taken up by cells. It is called “bad” cholesterol because, in excess, it can manifest as the plaque buildup that increases the risk for cardiovascular and other conditions associated with high cholesterol. In contrast, HDL is referred to as the “good” cholesterol because its function mitigates the negative impacts of cholesterol by clearing it out of the body. HDL transports cholesterol from other regions to the liver, where it is processed and removed, helping to keep arteries clear of cholesterol buildup. This is why having low HDL cholesterol can contribute to poor cardiovascular health and underlies a crucial distinction in the difference between LDL and HDL cholesterol for health outcomes. In short, you should aim for higher levels of HDL and lower levels of LDL. For those with familial hypercholesterolemia, it is typically the result of a mutation of one or more genes that encode LDL receptor cells in the liver, which can reduce the body’s cholesterol clearance rate. This is why certain individuals with genetic predisposition to high cholesterol can have elevated levels of bad cholesterol regardless of diet and other lifestyle and health factors.LDL: A cholesterol yardstick
A common way to gauge cholesterol risk is by LDL cholesterol levels. This value (LDL-C) can be calculated by what’s known as the Friedewald Equation, where you take your total cholesterol level as determined by a blood test (see Cholesterol Test below) then subtract the level of HDL cholesterol (HDL-C) and the level of a less common subtype of cholesterol known as very low-density lipoprotein (VLDL-C). Simply put, the formula should look like this: Total cholesterol - HDL-C - VLDC-C = LDL-C According to the CDC, 31.7% of Americans have elevated levels of LDL-C. This puts them at twice the risk for heart disease compared to people with more normative levels of LDL-C.Medications
- Lipitor (atorvastatin)
- Crestor (rosuvastatin)
- Zetia (ezetimibe)
- Zocor (simvastatin)
- Flolipid (simvastatin)
- pravastatin
- Antara (fenofibrate)
- Fenoglide (fenofibrate)
- Lipofen (fenofibrate)
- Tricor (fenofibrate)
- Repatha
- lovastatin
- Prevalite (cholestyramine, cholestyramine light)
- Colestid (colestipol)
- Welchol (colesevelam)
- fenofibrate micronized
- Lopid (gemfibrozil)
- Livalo (pitavastatin)
- Nexletol
- Vytorin (ezetimibe / simvastatin)
- Nexlizet
- Trilipix (fenofibric acid DR)
- niacin ER
- Caduet (amlodipine / atorvastatin)
- Praluent
- fluvastatin
- Lescol XL (fluvastatin ER)
- Ezallor
- Zypitamag
- Atorvaliq
- Leqvio
- Altoprev
- Nikita
- Fibricor (fenofibric acid)
- Triglide
- Colestid Flavored
- questran light
- Lerochol
- Roszet (rosuvastatin / ezetimibe)
- Niacor
- Juxtapid
- Evkeeza
Related Conditions
Atherosclerosis
A disease of the arteries in which fatty plaque buildup in the inner walls of arteries leads to restricted blood flow....
Coronary Artery Disease
A disease caused by atherosclerosis, CAD refers to a narrowing of arteries that supply blood to heart muscles....
Peripheral Artery Disease
A condition caused by atherosclerosis, PAD refers to a narrowing of arteries that supply blood to your limbs....